For many generations, society has embraced the idea that pregnant women are “eating for two.”
That old adage is frequently invoked as mothers-to-be are encouraged to abandon restraint and overindulge in every food craving in the name of nutrition.
It might have been sound advice back in the 1950s. Back then, only 1 in 10 women was dealing with health issues related to being overweight.
But, times have changed. As a world leader in nutrition, LSU’s Pennington Biomedical Research Center scientists have studied prenatal nutrition and discovered eating-for-two is no longer a good mantra for modern moms.

Leanne Redman, Ph.D., director of the Reproductive Endocrinology and Women’s Health Laboratory
“Pregnancy is the threshold of the future health of both you and your growing baby,” explains Leanne Redman, Ph.D., director of the Reproductive Endocrinology and Women’s Health Laboratory at Pennington Biomedical.
“Since the 1990s, research has shown the amount of excess weight a woman gains throughout her pregnancy can increase her risk of poor pregnancy and birth outcomes,” Redman says.
In addition, a mother’s weight gain in pregnancy has a big influence on the future weight gain and obesity of her child. The Institute of Medicine makes it easy for moms to follow a color-coded system.
Physicians now spend time counseling women about maintaining a healthy weight throughout pregnancy to help moms avoid excessive weight gain, which can trigger gestational diabetes and other harmful complications for both mother and baby.
Yet, despite those efforts, the eating-for-two myth still persists.
As both a researcher and the mother of five beautiful children, Redman understands both the importance and the challenges of maintaining a healthy weight during pregnancy.
Based on both her research and personal experience, she offers answers to some of the most common questions about healthy pre-natal weight gain.

SO HOW MUCH WEIGHT SHOULD YOU GAIN IN PREGNANCY?
In 2009, the Institute of Medicine revised its guidelines (see graphic) regarding how much weight you should gain during pregnancy.
To interpret the weight gain guidelines, identify your body mass index (BMI) group. BMI is a simple calculation health care providers use to understand health risks. To calculate your current BMI, click here.
To figure out your ideal pregnancy weight gain, enter your weight at the time you became pregnant and your height. Once the calculator determines your BMI, look at the chart to determine your recommended pregnancy weight gain.
For example, a newly pregnant women with a BMI of 27.5 falls into the overweight category. Her advised weight gain is a total of 15 to 25 pounds or 0.5-0.7 pounds per week.
Though these recommendations have been published for nearly a decade, many women are unaware they exist.
Realistically, even that knowledge is no match for your body prompting you to eat constantly.
If you add three 300-calorie snacks to a typical pregnancy diet, it is quite easy to rack up an additional 900 calories a day.
In addition, calorie-dense foods with high sugar and fat content are readily available—at the grocery store, the office snack machine, family dinners and a million other places—making it harder to manage gestational weight gain.
It’s no surprise nearly half of all pregnant women exceed the Institute of Medicine’s pregnancy guidelines.
But there are ways to keep you and your baby healthy.
For example: If you find you’re hungry, the best strategy is to keep small portions of protein-rich foods such as yogurt, meal replacement shakes or bars, a boiled egg or whole grain snacks on hand to curb appetite and quell cravings.
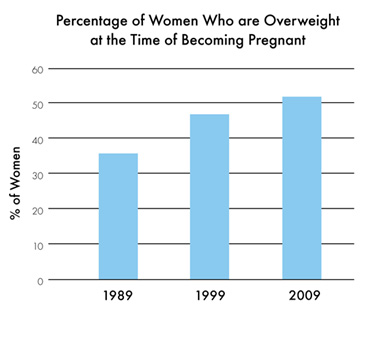
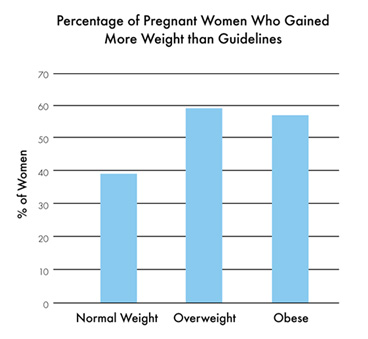
Women who are overweight or obese at the time of becoming pregnant are at a greater risk of gaining more weight. In 2009, about 39% of normal-weight women and 50% of overweight women. The report shows 59% of overweight women and 56% of obese women gained more weight than recommended.
HOW CAN YOU STOP UNWANTED WEIGHT FROM SNEAKING UP ON YOU?
Besides eating healthy and exercising regularly, many large clinical trials have shown the easiest and best tool for successful weight gain is self-monitoring.
Rather than being intimidated, make friends with your scale and pedometer! Women who track their progress—by counting calories, steps or weight gained—are the most successful at managing body weight.
The Institute of Medicine makes it easy for moms to follow a color-coded system.
If your pre-pregnancy BMI puts you in the normal weight category, follow the green zone for healthy gestational weight gain. If you’re in the overweight category, follow the orange zone instructions to keep your weight in the healthy range.
For information about women’s health research studies, click here.